Of patients that are infected with COVID-19 between 0.3% and 0.6% develop acute respiratory distress syndrome (ARDS) severe enough to need a mechanical ventilator. These patients will die if a ventilator is not available to treat them. As the pandemic surges in various locations around the world and as restrictions are eased, it is likely that the number of patients needing a ventilator will exceed the supply of traditional, full-featured, ventilators. Thus, many thousands to millions of lives can be saved by a simple ventilator that can be built quickly with off-the-shelf or easily fabricated parts.
An emergency-response ventilator must be simple, low-cost, and easy to assemble. At the same time it must provide at least the features needed to treat the majority of COVID-19 patients. This includes at a minimum the ability to precisely meter air flow and volume while regulating maximum pressure. Emergency ventilators that cannot regulate both flow and pressure are inadequate to meet the need.
The following figure shows why it is critical to regulate both flow and pressure when treating COVID-19 patients. The lungs of these patients often have very low compliance and hence pressure can build rapidly as air is pumped into the lungs. The figure shows the flow and pressure for settings of 300mL tidal volume, I:E of 1:2, and a respiratory rate of 15 on a simulated lung with low compliance. Maximum pressure is programmed to 40 cm H2O. The ventilator starts by regulating flow at 225mL/s to achieve the programmed tidal volume. Pressure, however builds rapidly and the flow must be curtailed at about 450ms to avoid exceeding maximum pressure. Pressure is then regulated at 40 cm H2O for the remainder of the inspiratory period. A ventilator that simply delivers a fixed flow or volume would exceed the maximum pressure here, possibly harming the patient. It could cut off when hitting maximum pressure, but then the patient would not receive enough oxygen. It is critical to precisely regulate both flow and pressure.
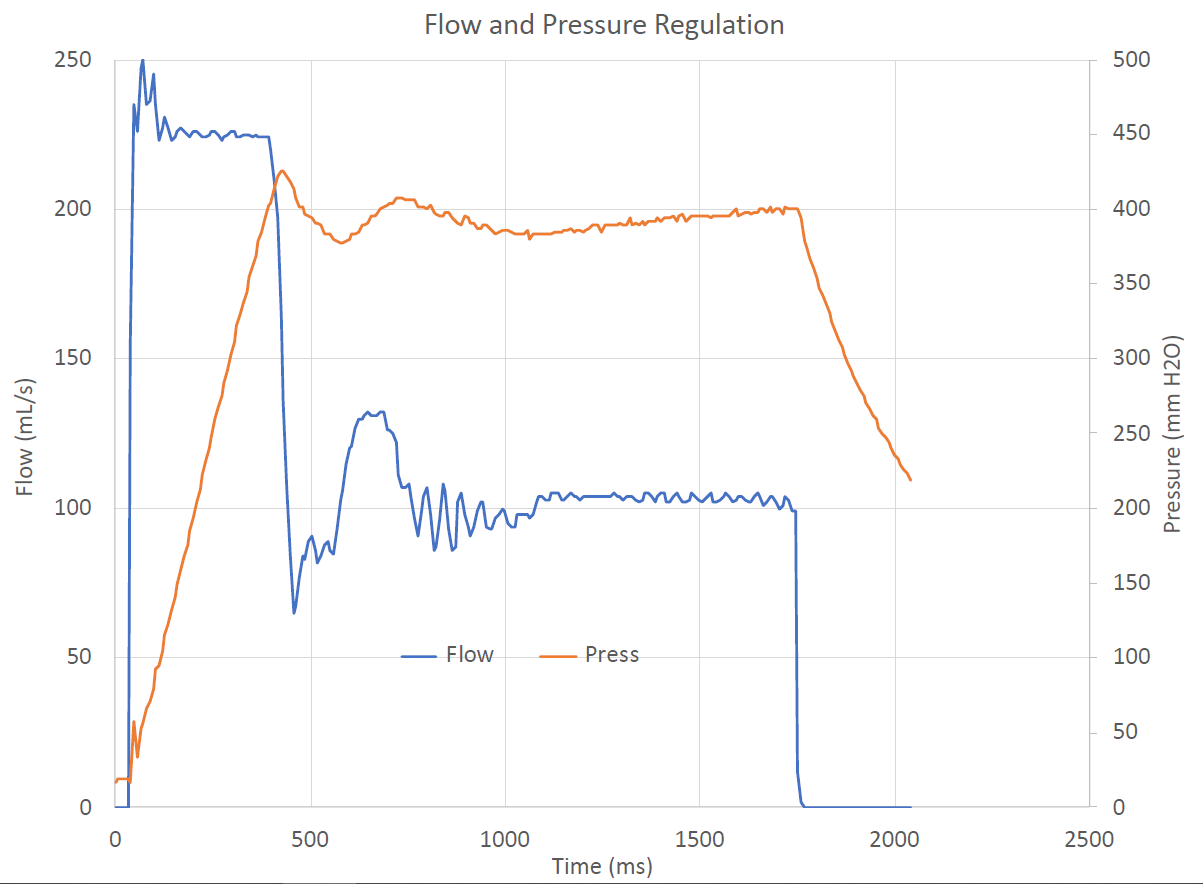 Figure: Flow and pressure control on a lung simulator
Figure: Flow and pressure control on a lung simulator
COVID-19 patients require FIO2 (fraction inspired oxygen) anywhere from 21% (normal air) to 100% (pure oxygen). In hospitals where oxygen blenders are avaialble, this mixing can be done external to the ventilator and the single-gas version of op-vent can be used. If an oxygen blender is not readily available, the blending version of op-vent can be used to precisely mix air and oxygen within the unit.
This report describes such a ventilator that at its heart contains just two key components – a proportional solenoid valve and a microcontroller – yet it meets all of the requirements needed to care for COVID-19 patients. It precisely regulates both volume and pressure. It supports spontaneous breathing modes. It can be optionally configured to blend a precise mixture of air and oxygen.